trending topics
market reports
-

Registration Now Open: MEDICAL JAPAN 2026 OSAKA – Western Japan’s Largest Healthcare Trade Show
2026-02-10
-

MEDICAL JAPAN 2025 OSAKA Returns to Showcase Global Innovations
2025-02-17
-

Visit MEDICAL JAPAN 2023 TOKYO and take full advantage of the business opportunities!
2023-09-01
-

US to distribute 400 million free N95 masks at CVS, Walgreens in COVID fight
2022-01-21
-

Ethiopia receives additional 2.2 mln doses of Chinese-donated COVID-19 vaccines
2022-01-21
-
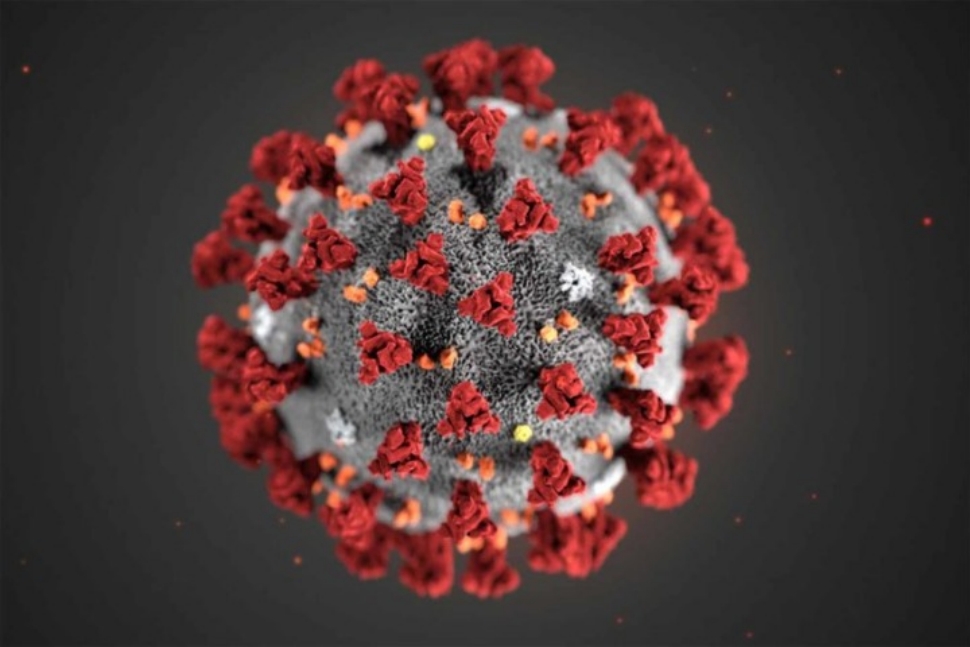
Hong Kong researchers say they develop novel material able to kill COVID-19 virus
2022-01-14
-

10 million more Chinese doses on way for Kenya
2022-01-14
-

Sino-African ties on track for a brighter future
2022-01-07
-
Efforts urged to boost COVID-19 vaccine production capacity in poor countries
2022-01-07
-
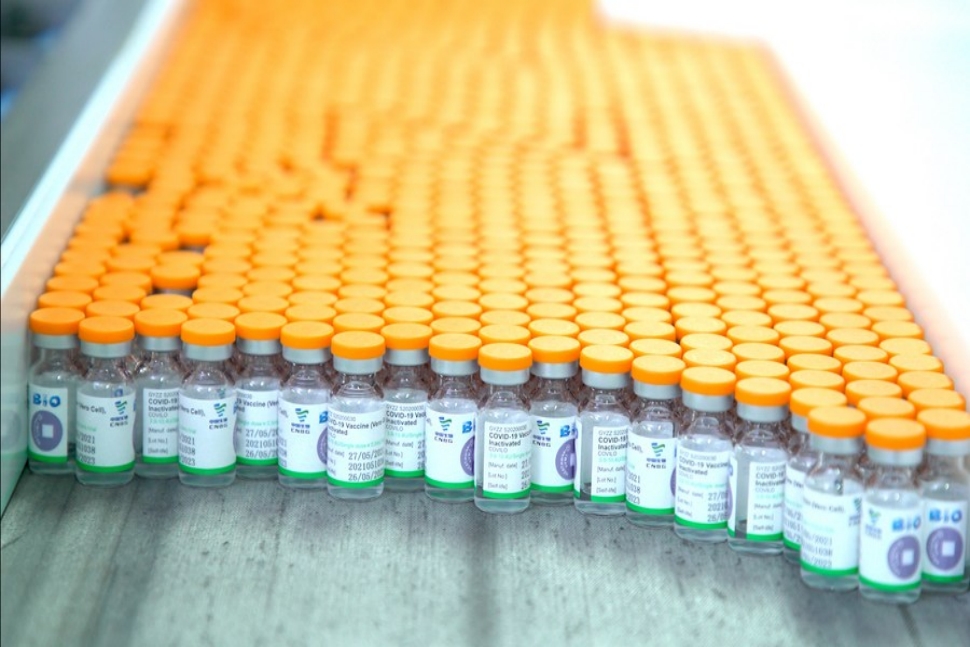
UAE approves Sinopharm's new protein-based COVID-19 vaccine
2022-01-07
United States is falling behind in the health care of older population, study shows
2020-11-04
An international study led by UCLA Fielding School of Public Health researchers has determined that the United States is far from the most effective healthcare provider for those 50 and older among 23 countries, ranging from Austria to the United States.
In terms of best practices, such as an annual doctor's check-up, the U.S. came in at 7thplace, with almost 8.5% of the over-50 population not seeing a doctor in 2016, the year that was surveyed. By contrast, a significantly higher percentage of older people in the Czech Republic, Belgium, France, Germany, Luxembourg, and Portugal than Americans got to see a doctor, with the shortfall ranging from roughly 5% in the Czech Republic to 7% in France.
"In the highest-performing health systems such as those of the richer countries of Western Europe, older adults almost all were able to consult a doctor, at least annually, without incurring high out of pocket expenses. That is not as common an outcome in the U.S."
James Macinko, UCLA Fielding School of Public Health professor in the departments of Community Health Sciences and Health Policy and Management
The study was published in the November edition of the peer-reviewed journal Health Affairs, and includes authors from universities in the U.S. and Brazil. The researchers' work examined some 100,000 older adults in one of the largest studies ever investigating cross-national differences in health care access, use, and related health expenditures among older adults, and one of only a handful that has investigated health system factors.
The countries surveyed include the U.S. and several with comparably high per capita incomes, including Luxembourg, Switzerland, Denmark, Sweden, Austria, Germany, and France, most of which have some variant of universal health coverage.
Not all the team's findings reflected poorly on the U.S. system, especially when it came to access to doctor visits. The access to care provided by the U.S. healthcare system comes with a price, however, researchers found. When it came to "catastrophic healthcare expenditures" (defined as when 25% or more of household income had to be spent out of pocket on health care), the U.S. ranked last in terms of high-income countries, although higher rates were observed in Eastern European and middle-income countries such as Brazil and Mexico.
"Even though catastrophic expenses in the U.S. are higher than in other comparable high-income countries, they affect only about 3% of the U.S. population aged 50 and over," said study co-author Flavia Cristina Drumond Andrade, an associate professor in the School of Social Work at the University of Illinois. "This is perhaps as a result of higher average income levels and the fact that in the U.S., adults ages 65 and older have access to a national health insurance program (Medicare), and additional coverage options are available to help defray costs through Medigap, employer-sponsored insurance, or Medicaid."
The researchers found that after individual characteristics and health needs were controlled for, national rates varied up to tenfold for poor access (no doctor visit) and threefold for potential overutilization (15 or more doctor visits and multiple hospitalizations) in the past year.
In terms of hospitalization, the U.S. had the highest number of older patients hospitalized, with more than 9 percent hospitalized two or more times in the past year, as opposed to as few as 6.5 percent in Germany, 5.5 percent in France, roughly 5 percent in Sweden and Switzerland, and a little over 4 percent in Denmark. A significant proportion of these events are re-hospitalizations that occur due to poor quality or inadequate follow-up care.
"Access to care remains a problem for 11 percent of all adults examined here, and in six countries, this figure reached or exceeded 15 percent," Macinko said. "There are numerous ways to enhance access, and all of these approaches may also strengthen the primary care basis of health systems such as using telemedicine for remote consultation and triage, employing community health workers for home care and control of some chronic disease risks, and guaranteeing access after-hours and on weekends to avoid relying on urgent care or hospital emergency departments, and these approaches could further enhance access, improve care coordination and integration for chronic conditions, and help contain health care expenditure growth."
UCLA Fielding School of Public Health
Journal reference:
Macinko, J., et al. (2020) Universal Health Coverage: Are Older Adults Being Left Behind? Evidence From Aging Cohorts In 23 Countries. Health Affairs.
doi.org/10.1377/hlthaff.2019.01570.
(news-medical)



 My Member
My Member Message Center
Message Center











